Explore additional AI-powered features to enhance your projects
JORIE AI SOLUTIONS
into Reality
Pretium malesuada enim, urna. Mauris nibh nec purus arcu, dapibus imperdiet id nibh. Nibh quisque elit interdum nulla. Consequat quam integer diam semper
We offer artificial intelligence-powered solutions that can be customized and retrofitted into your current infrastructure. This way we are able to maximize your outcome through optimization of your current resources.
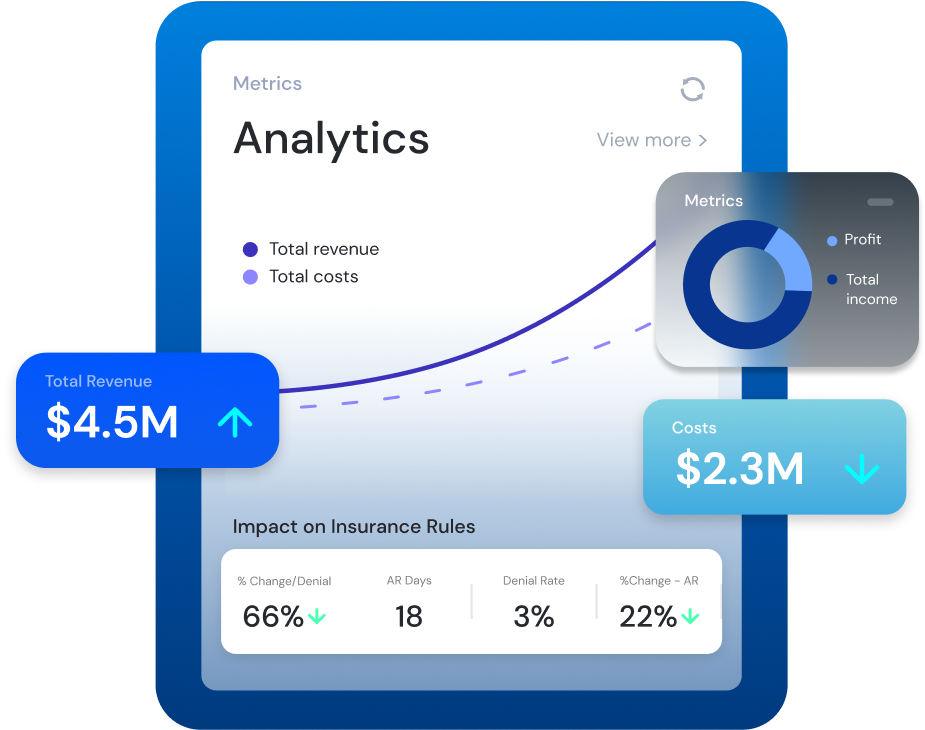

Jorie's RPA is the future of outsourced on-shore and off-shore Healthcare RCM. Our bots provide cost containment solutions that combine the latest AI and Robotic Process Automation (RPA) along with powerful BI Analytic Tools that produce reliable A/R profitability and reporting.
Jorie is the leading automated eligibility and benefits verification platform. With 300 eligibility checks a minute Jorie can verify eligibility and benefits instantly, with data that clients can trust. Reduces risks and saves you one - 700% faster than the competition.
Using advanced artificial intelligence pulls the patients data and uploads them directly into your HIS, reducing delays and reducing denials by 70%.

Our Jorie Bot is completely paperless. Manage and track your claims, faster than ever with our artificial intelligence. We’ve introduced industry leading claim status follow-ups that are 400% faster than the manual process.

Capturing charges with more efficiency. Our automated bot has over 150-man years of experience in RCM management. Making capturing charges easier than ever and fully automated with 99% accuracy and increasing your efficiency by 250%.
Powered by artificial intelligence, no more manually entering and approving thousands of payment transactions. Jorie’s automated payment posting is 6x faster. Jorie minimizes risk while maintaining and securing data, optimizing your cash flow, and saving you time.
We leverage your existing systems, wrapped in our best-of-breed technology & services to provide a platform for process excellence.
Explore additional AI-powered features to enhance your projects
•Customized automation tools to increase efficiency & results
•Smart learning tools - increase learning speed by over 40%
Navigating patients efficiently and effectively through the administrative process is a critical component of patient satisfaction and data accuracy.
For healthcare providers looking to grow top and bottom-line revenues and achieve price transparency, Jorie’s healthcare revenue cycle management experts offer charge master pricing services to ensure you have defensible prices and are charging appropriately to qualify for optimal episodic reimbursement.
For hospitals and health systems seeking to maximize revenues on specific services and improve their yields, Jorie’s healthcare revenue cycle management consultants can identify areas of opportunity to drive additional cash from operations on a sustained basis.
Jorie’s healthcare revenue cycle management experts use proven cash acceleration methodologies to help organizations quickly liquidate aging and at-risk accounts receivables into much-needed cash.
We can help you develop and implement a customized revenue cycle strategy and operating model that ensures patient satisfaction and internal span of control while boosting net revenues.

Welcome to Jorie AI, where our consulting services draw inspiration from industry leaders to redefine Healthcare Revenue Cycle Management. With a commitment to excellence and innovation, we tailor our approach to elevate your organization's financial outcomes.
• Evaluate Current State
• Identify Financial Gaps
• Diagnose Operational Challenges
• Analyze Revenue Performance
Technology Strategy and Planning
• Business Strategy Alignment with Technology
• Solution Cost/Benefit and Lifecycle Cost Analysis
• Technology Deployment Master
Technology Research & Development
• Technology Evaluation and Selection
• Proof of Concepts
Advanced Technology Integration
• Leveraging the latest in AI and RPA capabilities
• Optimizing workflows for increased productivity and efficiency
• Data management and integration
Technology Transformation
• Project Management
• 3rd Party Source Connectivity
Decision Support Systems
• Data Modeling
•Analytics/Decision Support
• Visualization Design
Technology Efficient. We utilize a combination of proprietary technologies and services to structure a seamless flow of critical patient data and financial information throughout your organization

